Rosacea affects roughly 16 million Americans, causing persistent facial redness, visible blood vessels, flushing, and (in some cases) acne-like breakouts. If you have tried topical creams and oral medications without satisfying results, you may be wondering whether IPL (intense pulsed light) can help control your rosacea symptoms.
The short answer is yes, for the right type of rosacea. IPL is one of the most well-studied and effective treatments for the vascular component of rosacea, including background redness, flushing, and visible broken capillaries. At Allen Medical Aesthetics in Des Moines, WA, we use IPL photofacial as part of a comprehensive approach to rosacea management. This guide explains exactly how IPL works for rosacea, which subtypes respond best, and what kind of improvement you can realistically expect.
IPL is an effective, well-studied treatment for rosacea-related redness and visible blood vessels. Most patients see 40% to 60% reduction in background redness and 60% to 80% improvement in visible broken capillaries after a series of 3 to 6 treatments. IPL works best for erythematotelangiectatic rosacea (subtype 1) and is less effective for papulopustular rosacea (subtype 2) or phymatous rosacea (subtype 3).
IPL targets the vascular (redness and blood vessel) component of rosacea. It does not cure rosacea, but it can significantly reduce visible symptoms and improve quality of life. Maintenance treatments are typically needed every 6 to 12 months.
How IPL Treats Rosacea
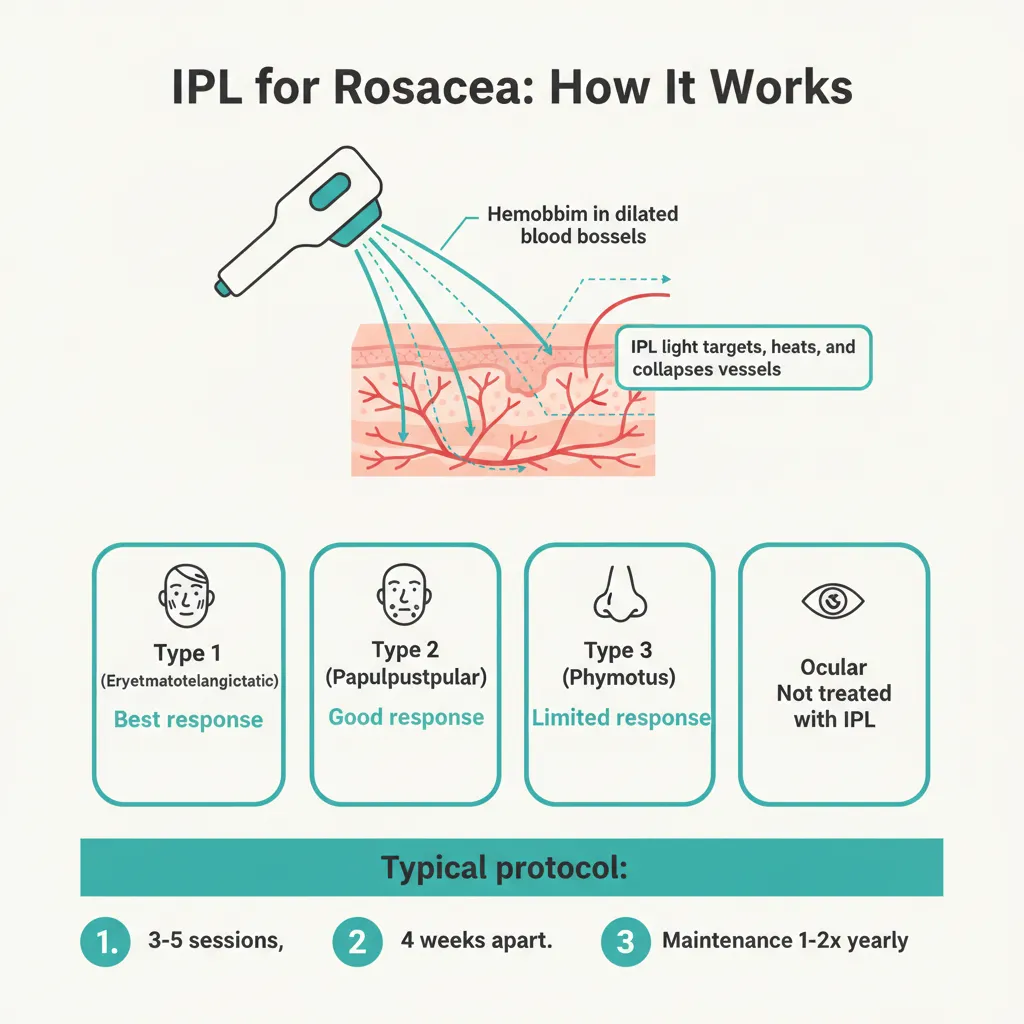
IPL works by delivering broad-spectrum light energy that is selectively absorbed by hemoglobin, the protein in red blood cells. When the light energy is absorbed, it heats the dilated blood vessels that cause rosacea redness. This thermal damage causes the vessel walls to collapse and seal shut. Over the following weeks, the body naturally reabsorbs the damaged vessels and the redness fades.
For background redness (the diffuse pink or red flush that many rosacea patients experience), IPL reduces the overall density of dilated capillaries near the surface of the skin. Even vessels that are too small to see individually contribute to this diffuse redness. By treating the network of superficial vessels across the cheeks, nose, chin, and forehead, IPL gradually calms the appearance of chronic flushing.
For visible telangiectasia (the individual broken blood vessels that appear as thin red or purple lines), IPL delivers enough energy to coagulate the vessel. The treated vessel darkens, constricts, and is gradually cleared by the immune system over 2 to 4 weeks.
IPL also has a mild anti-inflammatory effect. Studies have shown that repeated IPL treatments reduce the expression of certain inflammatory markers in rosacea-affected skin, which may contribute to longer-lasting symptom control beyond the vascular benefits alone.

“IPL is one of the most rewarding treatments I perform for rosacea patients. When you can visibly reduce that persistent redness and calm the flushing, it changes how people feel about their skin. I always tell patients that consistency is key, because each session builds on the last and the improvement really compounds over time.”
Morgan Selland, LME, LSO, MA Clinic Manager & Laser Safety Officer
Which Rosacea Subtypes Respond Best to IPL
Rosacea is classified into several subtypes, and IPL does not work equally well for all of them. Understanding your rosacea subtype is essential for setting realistic expectations.
Erythematotelangiectatic Rosacea (Subtype 1)
This is the subtype that responds best to IPL. It is characterized by persistent central facial redness, flushing episodes, and visible blood vessels (telangiectasia), primarily on the cheeks and nose. There are no papules or pustules.
Patients with subtype 1 rosacea typically see 40% to 60% improvement in background redness and 60% to 80% reduction in visible telangiectasia after a series of 3 to 5 treatments. Many patients report that their skin feels calmer, flushes less easily, and looks more evenly toned.
Papulopustular Rosacea (Subtype 2)
This subtype includes the redness of subtype 1 plus acne-like papules and pustules. IPL can help with the vascular component (redness and vessels), but it does not directly treat the papules and pustules. These inflammatory lesions are better managed with topical or oral medications.
For subtype 2 patients, a combination approach often works best. Topical treatments like metronidazole or ivermectin and oral antibiotics such as low-dose doxycycline can control the inflammatory component, while IPL addresses the underlying redness and vascularity. Active pustules should be treated and resolved before beginning IPL sessions.
Phymatous Rosacea (Subtype 3)
Phymatous rosacea involves thickening of the skin, most commonly on the nose (rhinophyma). IPL is not effective for this subtype. Phymatous changes require ablative treatments such as CO2 laser resurfacing, electrosurgery, or surgical reshaping.
Ocular Rosacea (Subtype 4)
Ocular rosacea affects the eyes and eyelids, causing dryness, irritation, and visible blood vessels on the eyelid margins. IPL has shown promising results for ocular rosacea in clinical studies, particularly for meibomian gland dysfunction. However, ocular IPL requires specialized protocols and eye protection, and should be managed in coordination with an ophthalmologist.
IPL is most effective for rosacea subtype 1 (redness and visible vessels without papules or pustules). If your rosacea includes inflammatory breakouts, those should be controlled with medication before starting IPL treatment.

Expected Improvement: What the Research Shows
Multiple clinical studies have demonstrated the effectiveness of IPL for rosacea. Here is a summary of the published evidence.
A 2005 study in Dermatologic Surgery followed 60 rosacea patients through a series of IPL treatments and found that 83% of patients showed significant improvement in redness and telangiectasia, with results maintained at 7-year follow-up for patients who received maintenance treatments.
A 2012 systematic review published in the British Journal of Dermatology analyzed 12 clinical studies and concluded that IPL produced statistically significant reductions in rosacea erythema and telangiectasia, with patient satisfaction rates consistently above 70%.
More recent studies (2019, 2020) have confirmed that IPL reduces not only visible symptoms but also measurable inflammation markers in rosacea skin, suggesting that the benefits extend beyond cosmetic improvement.
| Outcome Measure | Typical Improvement | Evidence Quality |
|---|---|---|
| Background Redness | 40% to 60% reduction | Strong (multiple controlled studies) |
| Visible Telangiectasia | 60% to 80% reduction | Strong |
| Flushing Frequency | 30% to 50% reduction | Moderate (patient-reported outcomes) |
| Patient Satisfaction | 70% to 85% report significant improvement | Strong |
| Quality of Life Improvement | Significant improvement on DLQI scores | Moderate to strong |
Questions about laser and skin?
Our providers offer consultations to discuss your options. The $50 fee is applied toward your first treatment.
Talk to a ProviderIPL vs Vascular Laser for Rosacea
Both IPL and vascular lasers (such as pulsed dye laser, or PDL) are effective for rosacea. They work on the same principle of targeting hemoglobin in blood vessels, but there are meaningful differences between the two approaches.
IPL delivers a broad spectrum of light wavelengths, which allows it to treat both superficial redness and visible blood vessels in the same session. It covers a larger treatment area per pulse, making full-face treatments faster. IPL is versatile and can address pigmentation concerns alongside redness in a single session.
Vascular lasers like PDL deliver a single, specific wavelength (typically 585 or 595 nm) that is highly targeted to hemoglobin. This precision makes PDL especially effective for individual, prominent telangiectasia and can treat deeper or more resistant vessels that IPL may not fully clear. However, PDL commonly causes purpura (bruising) that lasts 7 to 10 days, which is a significant cosmetic concern for many patients.
At Allen Medical Aesthetics, we offer both IPL photofacial and vascular laser treatment. For most rosacea patients, we start with IPL because it treats diffuse redness effectively, has minimal downtime, and does not cause purpura. If specific resistant vessels remain after the IPL series, vascular laser can be used to target those individually.
| Feature | IPL | Vascular Laser (PDL) |
|---|---|---|
| Wavelength | Broad spectrum (500 to 1,200 nm) | Single wavelength (585 or 595 nm) |
| Best For | Diffuse redness, multiple fine vessels | Large individual vessels, resistant telangiectasia |
| Downtime | Minimal (mild redness for hours) | Purpura (bruising) lasting 7 to 10 days |
| Sessions Needed | 3 to 6 | 1 to 3 |
| Pigment Treatment | Can treat brown spots simultaneously | Only targets vascular concerns |
| Discomfort | Mild (snapping sensation) | Moderate (rubber band snap with heat) |
For comprehensive rosacea management, IPL and vascular laser are not an either/or decision. Many patients benefit from starting with an IPL series for overall redness reduction, then using targeted vascular laser for any remaining stubborn vessels.
IPL Treatment Protocol for Rosacea
Treating rosacea with IPL requires a specific approach that differs from treating sun damage or general pigmentation. Rosacea skin is inherently sensitive and reactive, so conservative settings and careful technique are essential.
Before Treatment
Your provider will assess your rosacea subtype, skin type, and any current medications or topical treatments. Active inflammatory lesions (pustules or papules) should be controlled before beginning IPL. You will be asked to avoid sun exposure for 2 to 4 weeks prior to treatment and discontinue retinoids 3 to 5 days beforehand.
If you are using topical metronidazole, azelaic acid, or other rosacea medications, your provider will advise whether to continue or temporarily pause them around treatment sessions.
During Treatment
IPL for rosacea is typically performed with vascular-specific filters and conservative energy settings. The treatment starts at lower energy levels, with gradual increases based on your skin response. Each pulse of light feels like a quick snap against the skin, and the entire face treatment takes approximately 20 to 30 minutes.
Cooling gel or a built-in cooling system protects the epidermis and improves comfort. Your provider monitors the skin response in real time, adjusting settings as needed to ensure effective treatment without overtreating sensitive rosacea skin.
Treatment Schedule
The standard protocol for rosacea is 3 to 6 treatments spaced 3 to 4 weeks apart. Starting with lower energy at the first session allows your provider to gauge your skin response and adjust the protocol for subsequent sessions. Some patients with mild rosacea achieve satisfying results in 3 sessions, while those with extensive redness or numerous telangiectasia may need 5 to 6 sessions.
Maintenance and Long-Term Management
Rosacea is a chronic condition, which means it cannot be permanently cured. IPL can dramatically reduce visible symptoms, but ongoing management is necessary to maintain results. Without maintenance, redness and visible vessels gradually return over 6 to 18 months as new dilated vessels form.
Most rosacea patients benefit from maintenance IPL sessions every 6 to 12 months after completing their initial treatment series. The exact frequency depends on the severity of your rosacea and how quickly symptoms return.
Between IPL sessions, a comprehensive rosacea management plan should include daily mineral sunscreen (SPF 30 or higher), as UV exposure is a primary rosacea trigger. A gentle, fragrance-free skincare routine that avoids harsh exfoliants, alcohol-based products, and irritating active ingredients is essential. Topical prescriptions such as metronidazole, azelaic acid, or brimonidine can help maintain redness reduction between treatments.
Lifestyle Modifications That Support IPL Results
IPL treats the vascular symptoms of rosacea, but avoiding known triggers helps maintain your results longer and reduces the frequency of flare-ups. While triggers vary between individuals, the most common ones include the following.
- Sun exposure is the most common and most impactful rosacea trigger. Daily sunscreen and sun avoidance are non-negotiable for rosacea management.
- Temperature extremes, including hot showers, saunas, and cold wind, can trigger flushing. Lukewarm water and protective clothing help minimize episodes.
- Spicy foods and hot beverages are triggers for many rosacea patients. If these cause flushing for you, moderating intake can make a noticeable difference.
- Alcohol, especially red wine, is a well-documented rosacea trigger. Even moderate consumption can provoke flushing in sensitive individuals.
- Stress and intense exercise both raise core body temperature and increase blood flow to the face, potentially triggering a flare. Stress management and moderate exercise intensity can help.
- Harsh skincare products containing alcohol, fragrance, menthol, or strong exfoliating acids can irritate rosacea-prone skin. A simplified, gentle routine is always preferable.
IPL addresses the visible symptoms of rosacea, but trigger avoidance prevents new damage from forming. Combining IPL treatment with lifestyle modifications produces the most durable results.
Combining IPL with Other Rosacea Treatments
For patients with moderate to severe rosacea, a combination approach often delivers the best outcomes. IPL addresses the vascular component, while other treatments manage inflammation, skin barrier health, and surface texture.
DiamondGlow facial is an excellent complement to IPL for rosacea patients. The gentle exfoliation and hydrating serum infusion improve skin barrier function without the irritation that many rosacea-prone patients experience from traditional facials. DiamondGlow can be performed between IPL sessions to maintain skin health and hydration.
Topical prescription medications remain a cornerstone of rosacea management. Metronidazole (anti-inflammatory), azelaic acid (anti-inflammatory and anti-redness), and brimonidine (temporarily reduces redness by constricting blood vessels) can all be used alongside IPL therapy.
For patients whose rosacea includes a significant textural component, such as roughness or enlarged pores, treatments like gentle chemical peels (mandelic acid or lactic acid at low concentrations) can be introduced carefully after the initial IPL series has calmed the vascular component.
Frequently Asked Questions
How many IPL treatments does it take to see improvement in rosacea?
Most rosacea patients begin to see noticeable improvement after 2 to 3 IPL sessions. A full treatment series of 3 to 6 sessions, spaced 3 to 4 weeks apart, is typically needed for optimal results. Background redness improves gradually, while individual telangiectasia may clear after just 1 to 2 sessions.
Does IPL cure rosacea?
No. IPL significantly reduces the visible symptoms of rosacea (redness and broken blood vessels), but it does not cure the underlying condition. Rosacea is chronic, and new dilated vessels will gradually develop over time. Maintenance treatments every 6 to 12 months, combined with trigger avoidance and proper skincare, help sustain the improvement.
Can IPL make rosacea worse?
When performed by an experienced provider using appropriate settings, IPL should not worsen rosacea. However, overly aggressive settings, treating actively inflamed skin, or treating patients with darker skin tones can lead to adverse reactions. Starting with conservative settings and working with a provider experienced in rosacea management minimizes this risk.
Is IPL safe for all skin types with rosacea?
IPL for rosacea works best and is safest for Fitzpatrick skin types I through III (fair to medium skin). Patients with darker skin tones face a higher risk of hyperpigmentation or burns from IPL. Alternative treatments may be recommended for rosacea patients with skin types IV through VI.
How long do IPL results last for rosacea?
After completing a full treatment series, most patients maintain significant improvement for 6 to 18 months before redness gradually returns. Maintenance sessions every 6 to 12 months, combined with trigger avoidance and sun protection, help sustain results long-term.
Can I continue my rosacea medications during IPL treatment?
Most topical rosacea medications (metronidazole, azelaic acid) can be continued during IPL treatment, though your provider may recommend pausing them 1 to 2 days before and after each session. Oral antibiotics like doxycycline are generally safe to continue. Your provider will review your medication list and advise accordingly.
What does IPL feel like on rosacea-sensitive skin?
IPL feels like a series of quick, warm snaps against the skin. Rosacea patients may experience slightly more sensitivity than those without rosacea, but the discomfort is generally mild and brief. No anesthesia is typically required, and any redness or warmth after treatment resolves within a few hours.
Related Articles
This article supports our Ipl Photofacial service page. Learn more about treatment options, candidacy, and what to expect.

