If you have noticed tiny red or purple lines on your nose, cheeks, or chin that seem to appear out of nowhere, you are looking at broken blood vessels. Medically known as telangiectasia, these are small, dilated capillaries that sit just beneath the skin surface and become permanently visible. They are extremely common, especially as we age, and they are one of the concerns we treat most frequently at Allen Medical Aesthetics.
The good news is that broken blood vessels on the face respond exceptionally well to modern laser and light-based treatments. This guide explains what causes them, why they do not go away on their own, how treatment works, and what you can do to prevent new ones from forming.
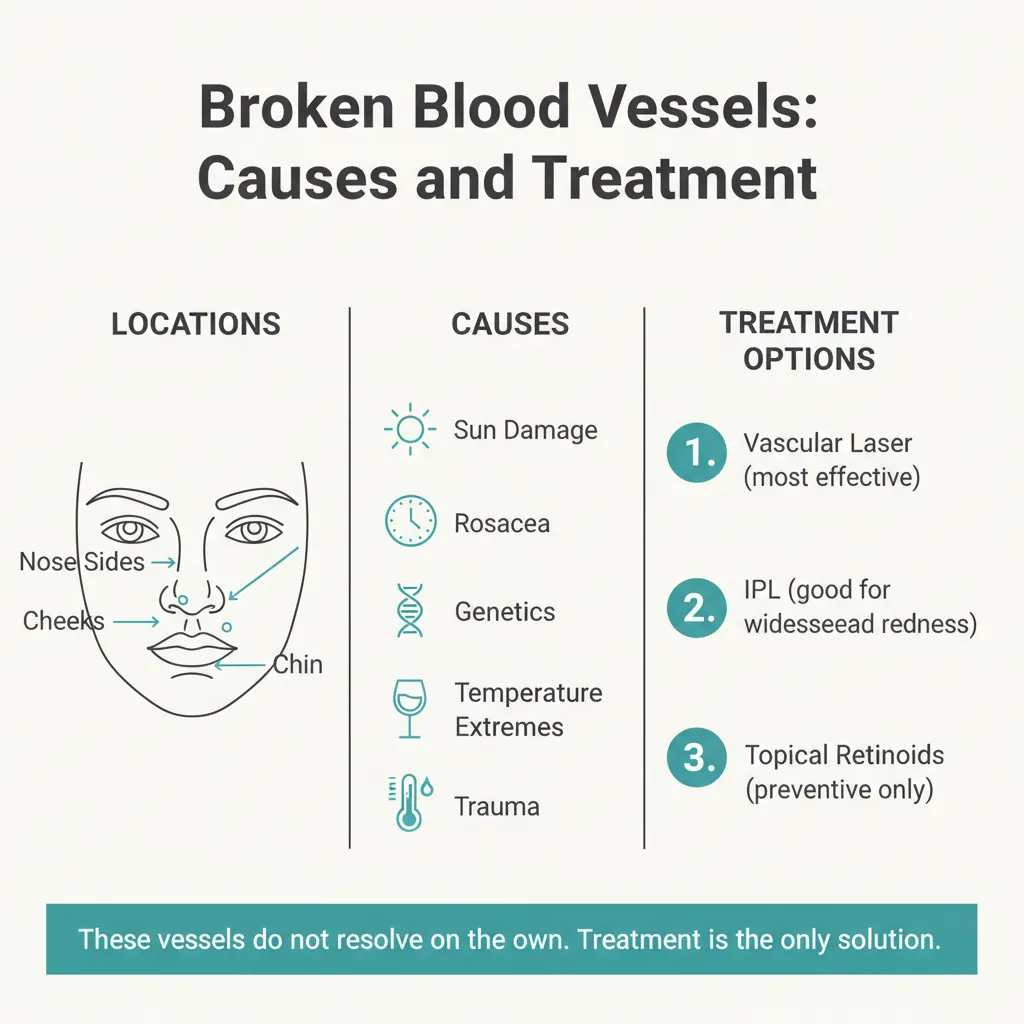
Broken blood vessels (telangiectasia) are permanently dilated capillaries that appear as thin red or purple lines on the face. Common causes include sun damage, rosacea, aging, and genetics. They do not heal on their own, but vascular laser treatment can eliminate them in 1 to 2 sessions with no downtime. Results are visible within 2 to 4 weeks.
Broken blood vessels on the face are permanent once they form. Vascular laser treatment is the fastest and most effective way to remove them. Most patients see significant clearance after just one session.
What Are Broken Blood Vessels?
The term "broken blood vessels" is actually a misnomer. These vessels are not broken in the traditional sense. They are capillaries and small venules that have permanently dilated (widened) beyond their normal size. Once dilated, the thin vessel walls cannot contract back to their original diameter, and the vessel becomes visible through the translucent surface layers of the skin.
Facial telangiectasias typically measure 0.1 to 1 mm in diameter and appear as fine, branching red or purple lines. They can occur as isolated individual vessels, clusters of small vessels in a web-like pattern, or diffuse networks that create an overall flushed appearance. They are most commonly found on the nose (especially the nostrils and nasal bridge), the cheeks, the chin, and around the eyes.
While broken blood vessels are almost always a cosmetic concern rather than a medical one, they can occasionally be associated with underlying conditions like rosacea that benefit from diagnosis and comprehensive treatment.
Common Causes of Broken Blood Vessels on the Face
Understanding what causes broken blood vessels helps you identify risk factors and take preventive steps. In most cases, multiple contributing factors work together over time.
Sun Damage
Chronic UV exposure is one of the primary causes of facial telangiectasia. Ultraviolet radiation breaks down the collagen and elastin that provide structural support to small blood vessels. Without this scaffolding, the vessel walls weaken and dilate. Sun damage also triggers an inflammatory response that can directly damage vessel walls. This is why broken blood vessels are especially common on sun-exposed areas like the nose and cheeks.
Rosacea
Rosacea is a chronic inflammatory skin condition that is strongly associated with broken blood vessels. The persistent inflammation and repeated flushing episodes that characterize rosacea cause progressive dilation of facial blood vessels. Over time, vessels that were only temporarily dilated during flushes become permanently expanded. Many patients first notice broken blood vessels as an early sign of developing rosacea.
Aging
As we age, the skin naturally thins and loses collagen. This makes existing blood vessels more visible and also reduces the structural support that keeps vessels at their normal diameter. The combination of thinner skin and weaker vessel walls means that broken blood vessels become more common with each decade, particularly after age 40.
Genetics
Some people are genetically predisposed to developing broken blood vessels. If your parents or close relatives have visible facial veins, you are more likely to develop them. Fair-skinned individuals (Fitzpatrick skin types I and II) are also more susceptible because their lighter skin provides less camouflage for dilated vessels.
Trauma and Pressure
Physical trauma to the face can rupture or permanently dilate small blood vessels. Common causes include forceful nose blowing, sneezing, vomiting, intense coughing, and facial injuries. Even aggressive facial scrubbing, manual extractions during facials, and the use of abrasive skincare devices can damage delicate facial capillaries. Chronic pressure (such as from wearing glasses that press against the nose) can also contribute.
Hormonal Changes
Estrogen affects blood vessel dilation and wall integrity. Pregnancy, oral contraceptive use, and hormone replacement therapy can all contribute to the development of broken blood vessels. This is one reason why facial telangiectasia is slightly more common in women than in men.
Environmental and Lifestyle Factors
Repeated exposure to extreme temperatures (both hot and cold), windburn, heavy alcohol consumption, and smoking all contribute to broken blood vessel formation. Alcohol causes repeated vasodilation that can become permanent over time. Smoking damages the blood vessel walls directly and impairs the skin's ability to repair itself.


“Broken blood vessels develop because the structural support around small capillaries weakens over time, whether from sun damage, rosacea, or natural aging. Once a vessel is permanently dilated, no topical product can reverse it. Vascular laser treatment is the definitive solution because it destroys the vessel itself, allowing the body to reabsorb it and redirect blood flow through healthy vessels.”
Tod Work, MSN, MPA, ARNP Medical Director & Medical Weight Loss Provider
Why Broken Blood Vessels Do Not Heal on Their Own
One of the most common questions we hear is whether broken blood vessels will eventually go away without treatment. Unfortunately, they will not.
Unlike a bruise (where blood leaks out of a vessel and is gradually reabsorbed), a broken blood vessel on the face is a structurally altered vessel that remains open and filled with blood. The vessel wall has permanently stretched beyond the point where it can contract back to its normal size. The smooth muscle cells in the vessel wall that would normally maintain tension are too damaged or weakened to close the vessel.
Topical creams marketed for broken blood vessels (including vitamin K creams, arnica, and various botanical extracts) cannot repair a structurally damaged vessel. They may temporarily reduce redness or inflammation in the surrounding skin, but they do not address the dilated vessel itself. The only way to eliminate a broken blood vessel is to destroy it so the body can reabsorb the tissue and redirect blood flow through healthier vessels.
Questions about laser and skin?
Our providers offer consultations to discuss your options. The $50 fee is applied toward your first treatment.
Talk to a ProviderTreatment Options for Broken Blood Vessels
Modern aesthetic medicine offers highly effective, non-invasive options for eliminating broken blood vessels on the face. The two primary approaches are vascular laser treatment and intense pulsed light (IPL).
Vascular Laser Treatment
Vascular laser treatment is the gold standard for removing broken blood vessels. The laser emits a specific wavelength of light that is absorbed by the hemoglobin (red pigment) inside the blood vessel. This absorption converts light energy to heat, coagulating the blood and causing the vessel walls to collapse. Over the following 2 to 4 weeks, the body's immune system clears the damaged vessel, and the visible line fades from view.
For facial broken blood vessels, pulsed dye laser (PDL) at 595 nm is the most commonly used and most effective option. It precisely targets superficial red vessels with excellent selectivity, meaning the surrounding skin is largely unaffected. Nd:YAG laser at 1064 nm may be used for deeper or larger vessels, or for patients with darker skin tones.
Most patients see significant improvement after a single laser session. Fine, superficial vessels often disappear immediately during treatment. Larger or deeper vessels may darken initially and then fade over 2 to 4 weeks. A second session may be recommended 4 to 6 weeks later to address any remaining vessels.
Intense Pulsed Light (IPL)
IPL treatment uses broad-spectrum light filtered to target blood vessels. While not as precisely targeted as a dedicated vascular laser, IPL offers the advantage of treating broken blood vessels alongside other concerns like sun spots, uneven pigmentation, and overall skin tone. This makes IPL an excellent choice for patients who want comprehensive facial rejuvenation rather than isolated vessel removal.
IPL typically requires 2 to 3 sessions for broken blood vessels and produces a more gradual improvement compared to vascular laser. It causes less bruising than PDL and has minimal downtime, making it a popular choice for patients who need to return to social activities quickly.
| Factor | Vascular Laser (PDL) | IPL |
|---|---|---|
| Precision | Very high, targets individual vessels | Moderate, treats broader area |
| Sessions for broken vessels | 1 to 2 | 2 to 3 |
| Bruising risk | Moderate (setting-dependent) | Low |
| Treats other concerns simultaneously | Primarily vascular | Yes (pigmentation, tone, texture) |
| Downtime | Minimal (possible bruising 7 to 10 days) | Minimal (mild redness for hours) |
| Best for | Prominent individual vessels | Diffuse redness plus vessels plus pigmentation |
What to Expect from Treatment
Whether you choose vascular laser or IPL, treatment for broken blood vessels is quick, comfortable, and requires no meaningful downtime.
A typical session takes 15 to 20 minutes. The skin is cleansed, protective eyewear is placed, and the laser or IPL device is applied to the treatment area. Each pulse feels like a quick, gentle snap with a warming sensation. Built-in cooling systems protect the skin surface and improve comfort. No topical numbing is needed for most patients.
Immediately after treatment, you may notice that treated vessels appear darker or slightly raised. This is a normal and expected response, and it indicates that the vessel has been successfully targeted. Mild redness and slight swelling around the treatment area may last a few hours. If PDL is used at purpuric settings, purple discoloration can last 7 to 10 days.
Over the next 2 to 4 weeks, the treated vessels gradually fade as the body clears the damaged tissue. Most patients see a dramatic reduction in visible broken blood vessels. A follow-up appointment allows your provider to assess results and determine if an additional session would be beneficial.
Apply mineral sunscreen daily after treatment and avoid hot showers, saunas, and intense exercise for 24 to 48 hours. These precautions help the treated vessels heal cleanly and reduce the chance of any prolonged redness.
Nose and Cheek Concerns
The nose and cheeks are the two most common locations for broken blood vessels on the face, and each area has characteristics worth understanding.
The nose has exceptionally thin skin with minimal subcutaneous fat, which makes even small dilated vessels highly visible. The nostrils and nasal bridge are particularly prone to broken blood vessels because they receive significant sun exposure, experience mechanical stress from nose blowing and glasses, and have dense networks of superficial capillaries. Broken blood vessels on the nose tend to be small and very responsive to laser treatment, often resolving in a single session.
The cheeks are prone to broken blood vessels from a combination of sun exposure, rosacea, and temperature fluctuations. Cheek vessels tend to appear in clusters or diffuse patterns rather than as isolated individual veins. Patients with rosacea-associated cheek redness often have a mix of visible individual vessels and background diffuse redness. Treatment may address the prominent individual vessels first, followed by broader treatment for the overall redness.
The chin and area around the mouth can also develop broken blood vessels, though less frequently than the nose and cheeks. These areas may be affected by hormonal changes, sun damage, or chronic lip licking and irritation.
Prevention: How to Protect Your Skin
While you cannot change your genetics or stop the aging process, several strategies can significantly reduce the rate at which new broken blood vessels develop.
- 1. Wear broad-spectrum sunscreen every day. SPF 30 or higher with zinc oxide or titanium dioxide protects against the UV damage that weakens vessel walls. Reapply every 2 hours during prolonged outdoor exposure.
- 2. Be gentle with your skin. Avoid harsh scrubbing, abrasive exfoliants, and aggressive facial devices. Pat your skin dry rather than rubbing. Choose soft washcloths and avoid pulling or stretching the facial skin.
- 3. Protect your face in extreme weather. Wear a scarf or balaclava in freezing temperatures and stay cool in extreme heat. Both temperature extremes trigger vasodilation that can become permanent over time.
- 4. Moderate alcohol consumption. Alcohol causes repeated dilation of facial blood vessels. Limiting intake reduces cumulative vascular stress.
- 5. Treat rosacea proactively. If you have rosacea, consistent management (topical medications, trigger avoidance, periodic vascular laser treatment) prevents the progressive vessel damage that leads to more visible broken blood vessels.
- 6. Avoid excessive heat exposure. Limit time in saunas, steam rooms, and very hot showers, especially if you are already prone to facial redness.
- 7. Do not pick or squeeze. Squeezing blemishes, blackheads, or whiteheads with excessive force can rupture capillaries and create permanent broken blood vessels.
When to See a Provider
Broken blood vessels are almost always a cosmetic concern, and the decision to treat them is personal. However, there are some situations where a professional evaluation is particularly worthwhile.
If you are developing new broken blood vessels frequently or in clusters, this may indicate an underlying condition like rosacea that would benefit from diagnosis and a comprehensive treatment plan. If broken blood vessels are accompanied by persistent facial redness, flushing episodes, or acne-like breakouts, a rosacea evaluation is recommended.
If you notice broken blood vessels appearing in unusual locations (not on the face), developing after starting a new medication, or accompanied by easy bruising or bleeding, mention these to your primary care provider. In rare cases, widespread telangiectasia can be associated with systemic conditions that warrant further evaluation.
For most patients, the right time to seek treatment is simply when the broken blood vessels bother you enough that you want them gone. There is no medical urgency, but there is also no reason to wait. Treatment is quick, effective, and safe.
Frequently Asked Questions
Can broken blood vessels on the face go away naturally?
No. Once a blood vessel has permanently dilated, it will not return to its normal size on its own. Topical creams and home remedies cannot repair a structurally altered vessel. Professional treatment (vascular laser or IPL) is required to eliminate visible broken blood vessels.
How many treatments do I need for broken blood vessels?
Most patients see significant improvement after 1 session with vascular laser. Fine vessels often disappear immediately, while larger vessels fade over 2 to 4 weeks. A second session may be recommended for any remaining vessels. IPL typically requires 2 to 3 sessions for optimal results.
Does treating broken blood vessels hurt?
Treatment is very well-tolerated. Most patients describe a mild snapping sensation similar to a rubber band. Sessions last about 15 to 20 minutes, and no numbing cream is needed for most treatments. Built-in cooling systems on the laser device protect the skin and enhance comfort.
Can broken blood vessels come back after laser treatment?
Treated vessels are permanently eliminated. However, new broken blood vessels can develop over time due to ongoing sun exposure, aging, rosacea, or other contributing factors. Consistent sun protection and gentle skincare habits slow the formation of new vessels.
Is laser treatment safe for broken blood vessels on the nose?
Yes. The nose is one of the most commonly and successfully treated areas. The thin skin of the nose allows the laser to reach superficial vessels very effectively. Most nasal broken blood vessels clear in a single session with minimal side effects.
What is the difference between broken blood vessels and spider veins?
The terms are often used interchangeably. Both refer to telangiectasia, which are dilated blood vessels visible through the skin. "Broken blood vessels" is the more common term for facial vessels, while "spider veins" is more often used for leg vessels or web-patterned clusters. Treatment is the same for both.
Can vitamin K cream fix broken blood vessels?
No. Vitamin K cream may reduce bruising or minor redness, but it cannot repair a permanently dilated blood vessel. Marketing claims about topical products eliminating broken blood vessels are not supported by clinical evidence. Laser or IPL treatment is the only proven method for removal.
Related Articles
This article supports our Vascular Laser Treatment service page. Learn more about treatment options, candidacy, and what to expect.

